Feline Ultrasound
A 12 year old, female spayed American Shorthair cat presented to Animal Imaging for an abdominal ultrasound after increased liver enzymes were noted on recheck bloodwork.
Veterinary Radiology Specialists
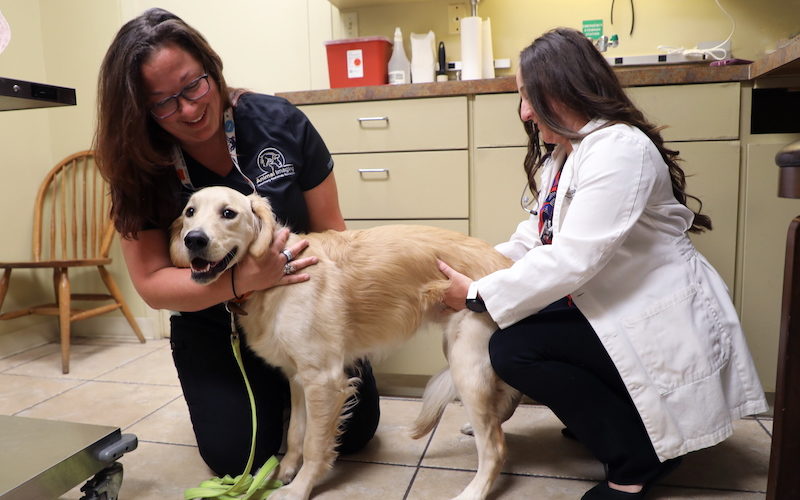
Our team treats our patients as if they were their own pet and will ensure they are as comfortable as possible during their visit.

Utilizing some of the most advanced equipment and technology available, our board-certified doctors are able to see abnormalities, clarify findings, and provide a detailed report in a timely manner.
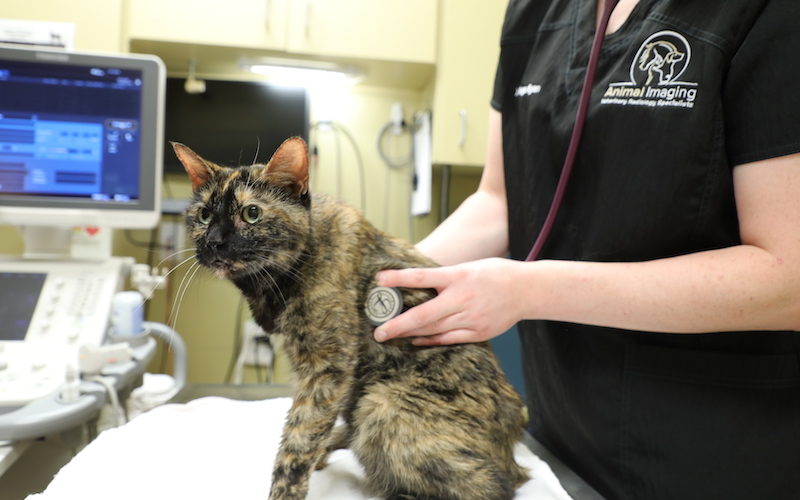
Being veterinarian owned allows us to stay unbiased in our commitment to providing the best specialty care available for our patients. Fast and accurate diagnostic imaging without bias.
At Animal Imaging, we value and care about our veterinarians and staff as much as we do for our patients and it shows in our collaborative and supportive work environment. Want to join our growing team?
A 12 year old, female spayed American Shorthair cat presented to Animal Imaging for an abdominal ultrasound after increased liver enzymes were noted on recheck bloodwork.
See the transformation of 5-year old Golden Retriever, Jetta as she goes from suffering with arthritis pain to playing and racing around the backyard once again!
A 10 year old neutered male Domestic Shorthair cat was referred to Animal Imaging for a thyroid scintigraphy and radiographs prior to radioactive iodine therapy.
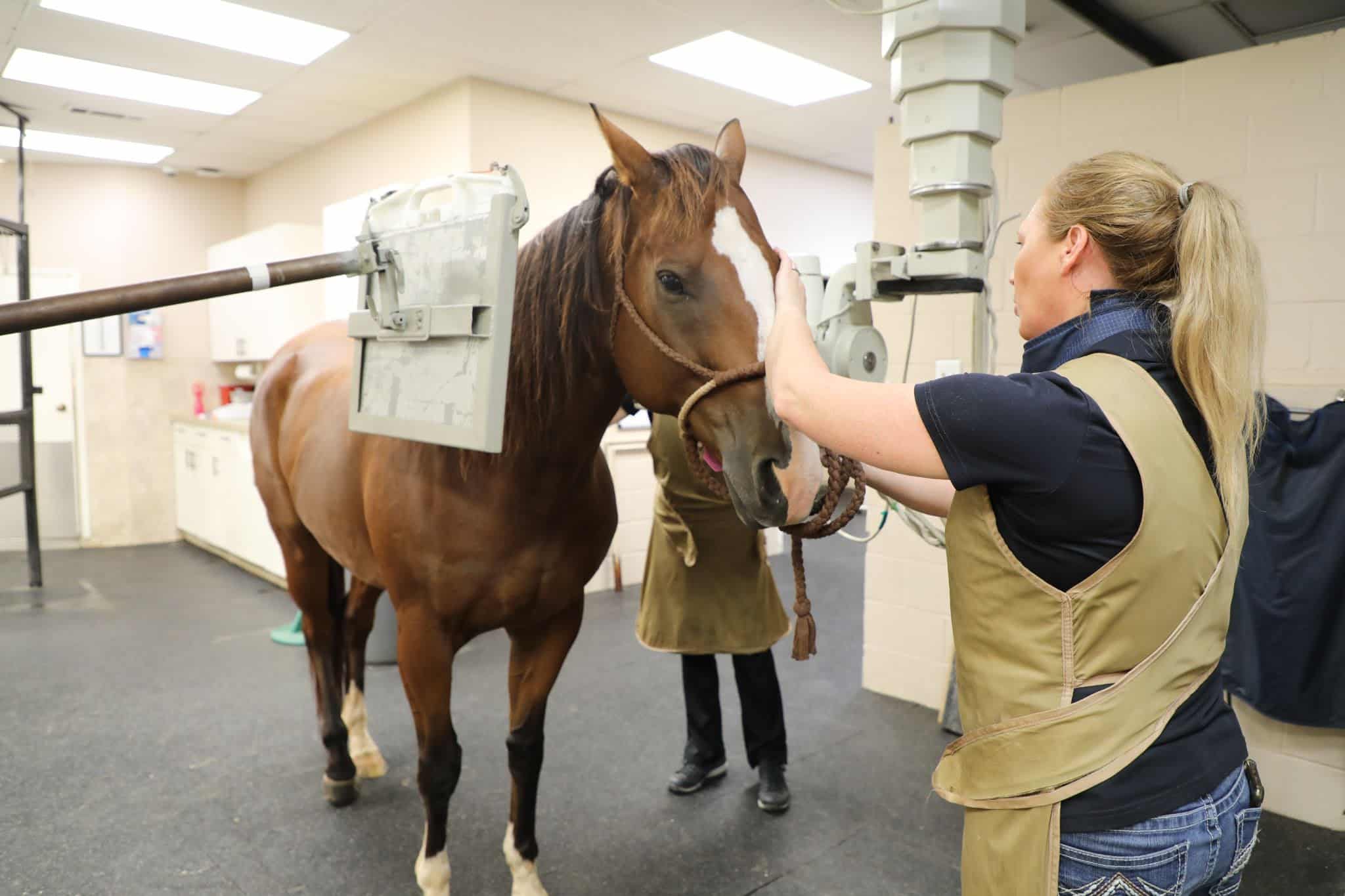
A two year old Quarter Horse mare was referred to Animal Imaging for a back-half bone scan.
Enter your email to be the first to hear about the latest case studies, announcements, and upcoming exclusive CE events.